Does a sharp, burning pain shoot from your lower back down through your buttock and leg?
Sciatica — the sciatic nerve is being compressed or irritated.
Every cough or sneeze sends an electric bolt down your leg. Sitting for long stretches only makes it worse, and one entire leg feels numb or pulled tight. This pain travels along a nerve, not just through a muscle.
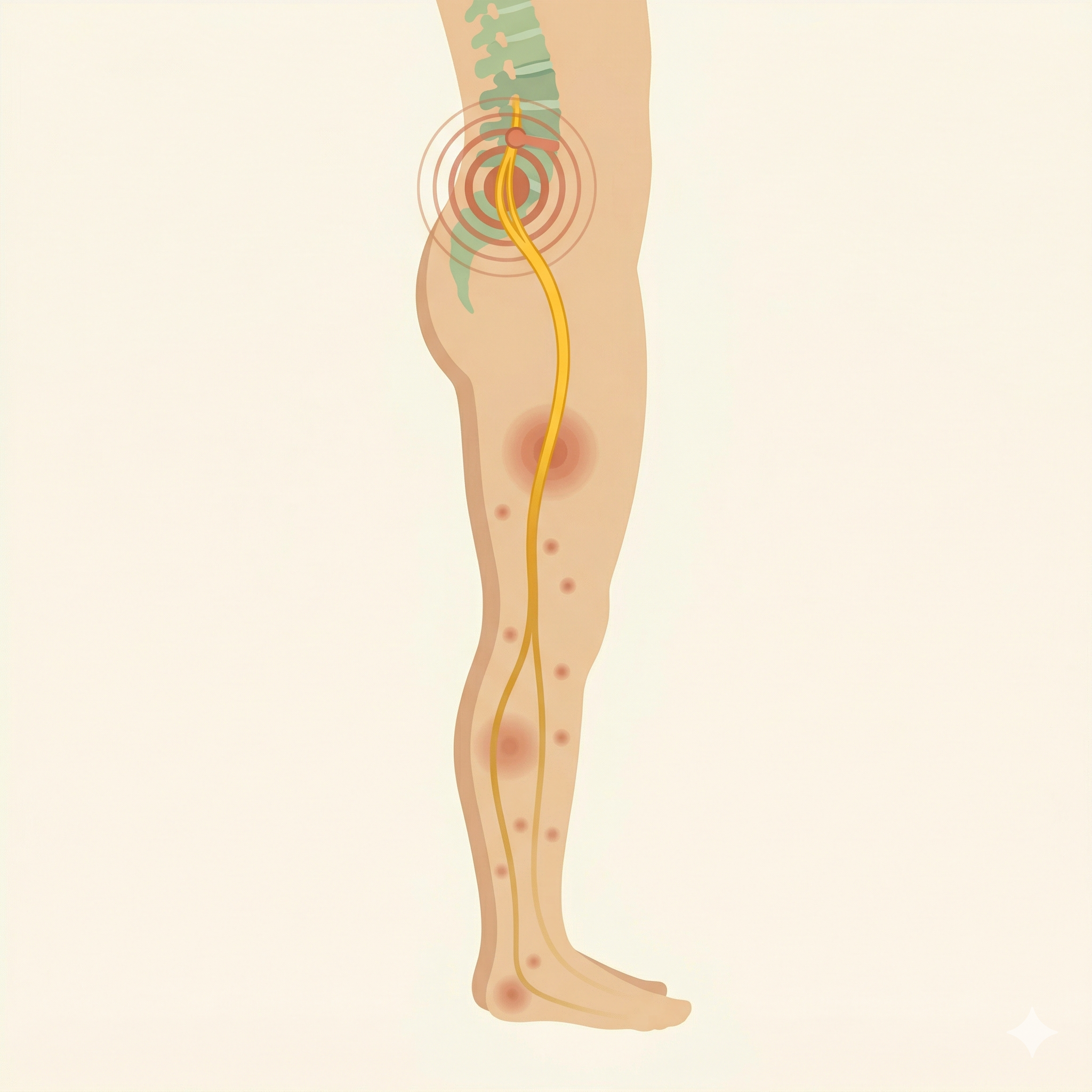
Quick Answer: The sciatic nerve is the longest nerve in the body, running from the lower back through the buttock, thigh, and calf all the way to the foot. Compression or irritation anywhere along this path produces pain, numbness, and pulling sensations throughout its entire length. Common causes include disc herniation, spinal stenosis, and piriformis muscle tightness. When the nervous system becomes sensitized (Alarm), even mild compression can produce severe symptoms.
Seek immediate medical attention if you have:
- Bladder or bowel dysfunction (incontinence or inability to urinate)
- Symptoms in both legs simultaneously
- Sudden significant weakness in the foot or toes
3 Key Points on This Page
- What sciatica is and why it radiates all the way to the foot
- How to tell which structure is compressing the nerve — disc, stenosis, or piriformis
- Managing sciatica through Circulation Therapy
Signs that suggest sciatica
- Radiating pain from buttock down the leg — The buttock and back of the thigh hurt more than the lower back itself, with pain shooting downward.
- Worsens with coughing, sneezing, or straining — Increased abdominal pressure amplifies nerve irritation, causing sudden sharp pain.
- Primarily on one side — Symptoms typically follow one leg rather than both.
- Worsens with prolonged sitting — Sitting increases pressure on the nerve, intensifying numbness over time.
- Numbness in the foot and toes — Tingling or numbness extends beyond the calf into the foot and individual toes.
What causes sciatica?
Sciatica is not a diagnosis in itself — it describes a symptom pattern of pain along the sciatic nerve. The cause depends on where the nerve is compressed.
- Lumbar disc herniation — The most common cause. A bulging disc presses on the sciatic nerve root in the lower back.
- Spinal stenosis — Narrowing of the spinal canal squeezes nerve roots.
- Piriformis tightness — The piriformis muscle, deep in the buttock, directly compresses the sciatic nerve as it passes nearby.
Alarm × Load Framework
Even with nerve compression (Load), symptoms can remain mild if the nervous system is calm. Conversely, when the nervous system is sensitized (Alarm) by stress, poor sleep, or prior pain, even slight compression can cause severe symptoms.
→ Addressing nerve compression alone is not enough. Calming nervous system sensitization must happen in parallel.
Our Approach at Yonsei SM Pain Clinic
For sciatica, the key is to pinpoint where the nerve is compressed and improve the environment around it.
- Phase 1: Calm Down
Reduce tension and inflammation around the nerve. Hydrodissection (Circulation HD) creates space around the compressed nerve and restores nerve glide. Lowering nervous system sensitization stabilizes the hypersensitive state. - Phase 2: Wake Up (Circulation PT)
Neural gliding exercises restore flexibility to the sciatic nerve. Strengthening the gluteal muscles and core distributes load away from the nerve. Movement correction reduces repetitive stress on the nerve pathway. - Phase 3: Connect
Correct sitting posture and walking patterns. Gait analysis identifies movement habits that overload the nerve, then guides you to eliminate them in daily life.
Frequently Asked Questions
Is sciatica the same as a herniated disc?
Sciatica describes the symptom — radiating pain down the leg — while disc herniation is one possible cause. Spinal stenosis and piriformis tightness can produce identical symptoms. Disc Herniation →
Does all leg numbness mean sciatica?
Leg numbness can also stem from peripheral nerve issues, vascular problems, and other causes. The distribution of numbness and which movements change it are important clues for differentiating the cause. Leg Numbness Q&A →
Why does sitting make it worse?
Sitting stretches the piriformis and increases disc pressure, amplifying sciatic nerve compression. Standing and moving briefly every 30 minutes helps. Sitting Pain Q&A →
Will sciatica resolve on its own?
Mild cases sometimes improve with time. However, if symptoms persist beyond three months or continue to worsen, active assessment and treatment are warranted. Treatment Duration Q&A →
Can I exercise during treatment?
Walking and gentle stretching within pain-free limits are helpful. High-impact activities and aggressive forward-bending should be avoided. Movement correction is integrated into each treatment phase. Back Exercise Q&A →
References
- Koes BW, et al. Diagnosis and treatment of sciatica. BMJ. 2007;334(7607):1313–1317. PMID 17585160
- Stafford MA, et al. Sciatica: a review of history, epidemiology, pathogenesis, and the role of epidural steroid injection in management. Pain. 2007;124(1–2):5–25.
- Lewis RA, et al. Comparative clinical effectiveness of management strategies for sciatica. Spine J. 2011;11(2):150–158.
- Haugen AJ, et al. Prognostic factors for recovery in patients with sciatica: a systematic review. PM&R. 2012;4(2):118–128.
Related Articles
Pain shooting down your leg? We’ll find the source.
Nerve pathway assessment and gait analysis help us build a targeted treatment plan.
Book Online