Is your back pain worse when standing or walking — and relieved when you sit or bend forward?
Spinal Stenosis — narrowing of the spinal canal pressing on nerves.
You can only walk a short distance before your legs feel heavy and numb — and you have to stop. But sitting down or leaning forward brings quick relief. Cycling may feel fine, yet walking is a struggle. This pattern points to spinal stenosis.
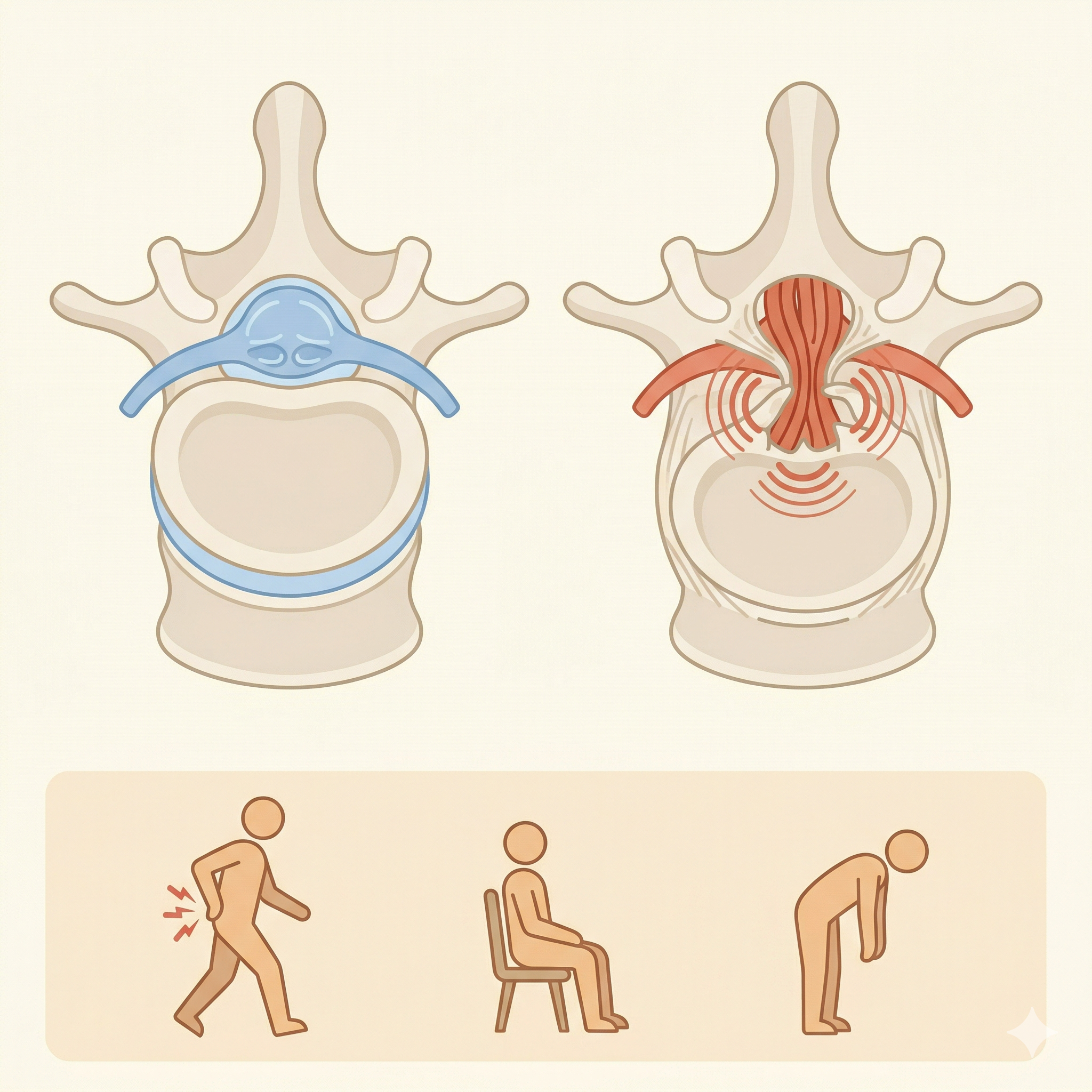
Quick Answer: As the spinal canal narrows, the nerves inside become compressed — a condition called neurogenic claudication. Walking demands more blood supply to the nerves, but a stenotic canal cannot deliver it, triggering pain and numbness. Sitting or bending forward widens the canal momentarily, restoring blood flow and bringing fast relief. Unlike disc herniation, bending forward feels better in stenosis. Nerve sensitization (Alarm) often determines how intense symptoms are — independent of how much narrowing the MRI shows.
Seek immediate medical attention if you have:
- Bladder or bowel dysfunction (urinary incontinence, inability to urinate)
- Weakness or paralysis in both legs simultaneously
- Sudden inability to walk
3 Key Points on This Page
- Why walking triggers leg pain and resting relieves it (neurogenic claudication)
- How to tell spinal stenosis apart from disc herniation
- Conservative management through Circulation Therapy
Signs that suggest spinal stenosis
- Leg pain and numbness when walking, relief when resting (neurogenic claudication) — After a set distance, legs feel heavy or numb, forcing you to stop. A brief sit-down lets you walk again.
- Relief when leaning forward — Pushing a shopping cart or grocery trolley (slightly hunched) eases symptoms noticeably.
- Worsening when standing upright or bending backward — Straightening the spine or leaning back intensifies leg symptoms.
- Cycling remains possible — The seated, slightly forward-flexed posture on a bike often keeps symptoms at bay.
- Symptoms in both legs — Unlike disc herniation, numbness can affect both legs, not just one.
What is spinal stenosis?
The spinal canal is the tunnel through which the spinal cord and nerve roots travel. With age, bones, ligaments, and discs gradually thicken and deform, shrinking this tunnel. When narrowing compresses the nerves, blood supply to them becomes restricted, producing numbness and pain.
Walking increases the nerves’ demand for oxygen, but a stenotic canal cannot keep up. Sitting or forward-bending opens the canal slightly, blood flow recovers quickly, and symptoms subside.
Neurogenic vs. Vascular Claudication
- Neurogenic (stenosis) — Relief comes quickly with sitting or forward lean. Cycling is usually fine.
- Vascular (peripheral artery disease) — Relief is slower even when seated. Cycling also hurts.
Both can coexist, so accurate differentiation matters.
Why can severe stenosis on MRI sometimes cause mild symptoms?
Imaging findings and symptom intensity do not always match. Pain research shows that nerve sensitization (Alarm) plays as large a role as the physical compression itself (Load).
Load
Degree of canal narrowing and nerve compression — visible on MRI.
Alarm
Nervous system sensitization, stress, sleep quality, past pain history — not visible on imaging.
This is why reducing nervous system sensitization (the Calm Down phase) is essential alongside addressing the structural narrowing.
Our Approach at Yonsei SM Pain Clinic
For spinal stenosis, the goal is to improve the environment around compressed nerves and restore walking capacity.
- Phase 1: Calm Down (Circulation HD)
Reduce swelling and tension around the nerves. Hydrodissection creates space around compressed nerves and releases adhesions. Lowering nerve sensitization stabilizes the overreactive nervous system. - Phase 2: Wake Up (Circulation PT)
Activate weakened core and gluteal muscles. Stronger spinal support muscles reduce uneven loading on the narrowed segments. Gait training gradually extends pain-free walking distance through movement correction. - Phase 3: Connect
Optimize walking patterns. Gait analysis identifies the posture and stride length that minimizes nerve stress, and we guide you to apply these findings in everyday life.
Frequently Asked Questions
How is stenosis different from a herniated disc?
Disc herniation typically worsens when bending forward and improves when arching back. Stenosis is the opposite — forward bending relieves symptoms and standing upright worsens them. Both conditions can coexist, so careful assessment is essential. Disc Herniation →
Does spinal stenosis always require surgery?
Surgery is considered when bladder/bowel dysfunction or progressive paralysis is present. In many cases, conservative treatment — improving the nerve environment and strengthening surrounding muscles — restores walking capacity. Surgery Decision Q&A →
Should I walk for exercise?
Walking within a pain-free range is generally beneficial. When legs start to ache, sit briefly and then resume — gradually building distance. Pushing through pain is not recommended. Walking Pain Q&A →
Is cycling safe with stenosis?
Many stenosis patients find that the seated, slightly flexed position on a stationary bike reduces symptoms. Cycling can be a useful low-impact cardio option, though individual responses vary.
How long does treatment take?
This depends on the degree of narrowing, nerve symptoms, and muscle condition. Calming the nervous system and restoring muscle function proceed in sequence. Treatment Duration Q&A →
References
- Ammendolia C, et al. Nonoperative treatment for lumbar spinal stenosis with neurogenic claudication. Cochrane Database Syst Rev. 2013;(8):CD010712.
- Weinstein JN, et al. Surgical versus nonsurgical therapy for lumbar spinal stenosis. N Engl J Med. 2008;358(8):794–810. PMID 18287602
- Deyo RA, et al. Spinal-fusion surgery — the case for restraint. N Engl J Med. 2004;350(7):722–726.
- Fritz JM, et al. Lumbar spinal stenosis: a review of current concepts in evaluation, management, and outcome measurements. Arch Phys Med Rehabil. 1998;79(6):700–708.
Related Articles
Struggling to walk? Have your neurogenic claudication evaluated.
Gait analysis and nerve function assessment help us build a personalized treatment plan.
Book Online